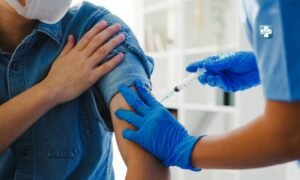
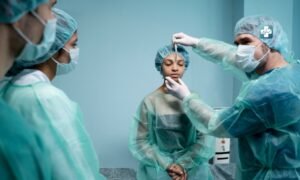
Medicine today looks less like top-down orders, more like listening to voices from the clinic floor. Picture this: real change begins when doctors and nurses help shape how things run. Instead of only managers calling shots, those treating patients join in planning. Think different – decisions shaped by hands-on experience often hit closer to reality. Leadership grows stronger when treatment knowledge meets budget choices without fighting each other. It’s not about new job labels stuck onto clinicians. Surprise – true impact comes when daily care wisdom guides long-term goals inside hospitals and clinics alike.
The Move to Empower Doctors and Nurses
Back in the day, doctors and managers hardly ever spoke the same language – like ships passing in the fog. Money mattered most to office planners; bedside care ruled for medical teams. Lately, though, something shifted. People who’ve worked directly with patients now step into decision-making spots. That change? It’s quietly breaking down old walls. Hospitals notice better teamwork and fewer errors when those calling shots have worn scrubs themselves. Real talk shapes policy more than rows of numbers ever could. Because leaders show real understanding, workers believe their struggles matter. When people sense that truth, new ideas start spreading quietly through the ranks. Problems stuck for years begin to shift, moved by fresh thinking rising from within.
Impact on Patient Outcomes and Quality of Care
The most compelling argument for this management style lies in the measurable results seen in patient recovery and safety statistics. A focus on clinical leadership ensures that quality improvement is not just a checkbox for accreditation but a lived value within the organization. Leaders with a background in care are naturally inclined to prioritize evidence-based practices and clinical outcomes over purely bureaucratic metrics. Because they have seen the consequences of medical errors or inefficient workflows firsthand, they are more motivated to implement rigorous safety protocols. This professional perspective allows for the identification of bottlenecks that a non-clinical manager might overlook, such as the nuances of nurse-to-patient ratios or the ergonomics of a ward layout. The result is a healthcare environment that is more responsive, more precise, and ultimately more humane for the individuals it serves.
Navigating the Challenges of Dual Expertise
Transitioning from a practitioner to a guide of an entire department or facility is not without its hurdles. Many professionals find themselves caught in a “identity tug-of-war” where they must balance their desire to treat patients with the necessity of attending board meetings and managing budgets. Mastering clinical leadership requires a specific set of soft skills that are not always taught in medical school, such as conflict resolution, strategic planning, and financial literacy. Organizations must therefore invest in robust training programs that help these individuals bridge the gap between their technical skills and their new administrative duties. The challenge lies in ensuring that these leaders do not lose their “clinical soul” as they become more entrenched in the machinery of hospital operations. Keeping one foot in the world of practice while the other moves toward policy is a delicate balancing act that requires resilience and a clear sense of purpose.
Future Horizons in Integrated Medical Governance
As we look toward the future, the role of clinical leadership will only become more vital as healthcare technology becomes more complex. With the integration of artificial intelligence and personalized medicine, we need voices at the top who can vet these technologies through a lens of ethics and efficacy. The future of healthcare is one where the hierarchy is flatter and the flow of information is more transparent. In this coming era, those who can navigate both the language of the laboratory and the language of the boardroom will be the architects of a more sustainable system. By championing this integrated approach, we ensure that the healthcare industry remains focused on its primary mission: the healing and well-being of the community. The journey toward this integrated model is ongoing, but the progress made so far suggests that when medical expertise leads the way, everyone from the surgeon to the patient stands to benefit.
Moving Forward with Visionary Care
The path to a more efficient healthcare system is paved with the insights of those who provide care every single day. As the industry continues to grapple with rising costs and an aging population, the necessity of clinical leadership becomes undeniable. It is no longer enough to simply manage a facility; we must lead it with a profound understanding of the human element at its core. By continuing to support and develop these hybrid professionals, we are investing in a future where the quality of care is never sacrificed for the sake of the process. The evolution of our institutions depends on our ability to merge clinical wisdom with strategic foresight, creating a legacy of excellence that lasts for generations.